Preparing for another synthetic cannabinoids spike
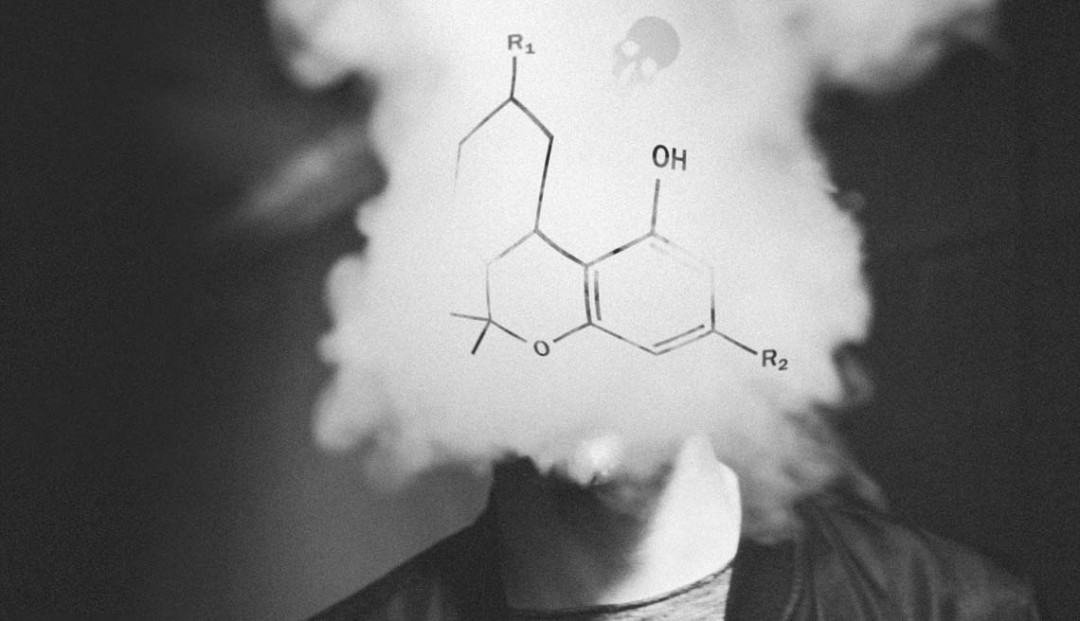
Spikes in synthetic cannabinoids harm can happen at any time, and we continue to see incidents that leave in their wake a trail of casualties. In October Tess Nichol talked with some of those who responded to a recent cluster of hospitalisations in Taranaki about what is being put in place.
As New Zealand was settling into warmer spring days, a dark cloud drifted into view. Reports of new analogues of deadly synthetic cannabinoid were worrying members of the network set up to respond to any surges of intense harms associated with drug use.
In September this year, it was reported that a particularly harmful strain, AMB-FUBINACA, was back, along with a new, unclassified but equally dangerous strain MDMB-4en-PINACA, an analogue of 5F-ADB which was responsible along with AMB-FUBINACA for the majority of synthetic cannabinoid deaths in New Zealand in 2017 and 2018, when more than 70 people died.
A wave of synthetic cannabinoid-related deaths made headlines in 2018, with many of those affected already very vulnerable - those sleeping rough have been the most impacted. The motivation to use these toxic substances is complicated. For some, it’s because these substances are cheap and provide a powerful, dissociative high. Others began using them to avoid workplace drug testing and have found it difficult to stop.
The only relationship between synthetic cannabinoids and cannabis plant material is that synthetic cannabinoids and the main active ingredient in the cannabis plant, THC, act on the same part of the brain (the cannabinoid system), to cause a psychoactive effect. However, the harm profile is dramatically different with synthetics potentially causing seizures, psychosis, organ damage and death.
Those involved in responding to the acute harm caused by synthetic cannabinoids are now focused on making sure we do not see a repeat of what happened two years ago. What they’ve learned from last time means the response will be faster and better coordinated, which will hopefully lessen the harmful impact on affected communities.
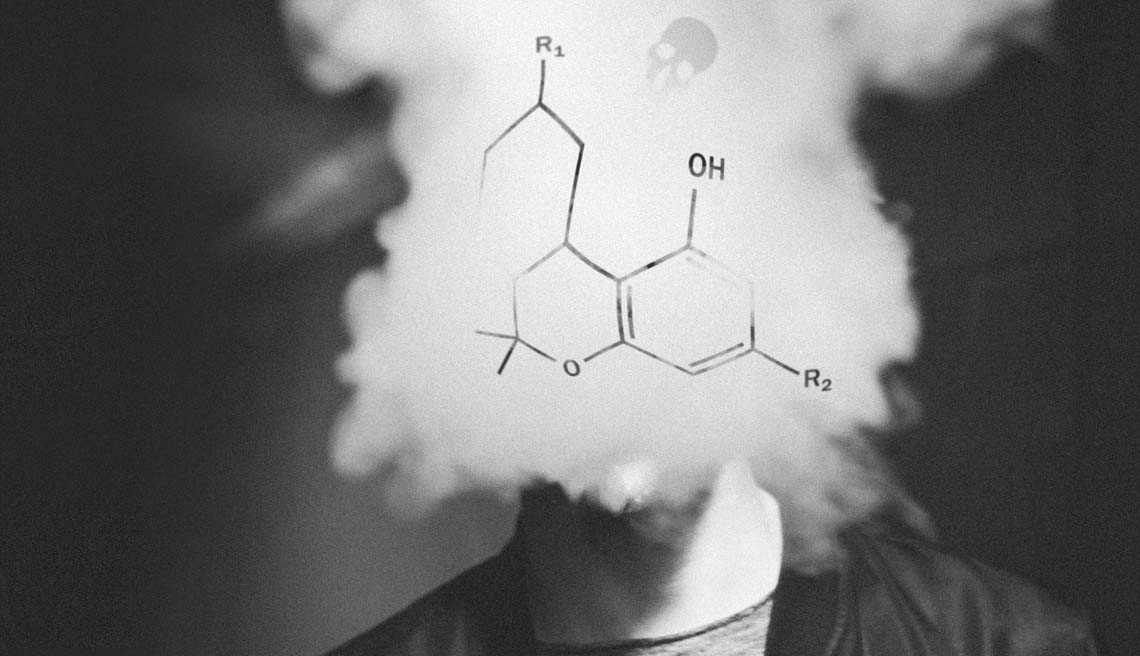
Chemical structure of AMB-FUBINACA, in a cloud of smoke which covers an unidentified person's head. - AMB-FUBINACA, is back, along with a new, unclassified but equally dangerous strain MDMB-4en-PINACA.
Ambulance, local health providers, the Drug Foundation, and government organisations are paying close attention to how and where synthetics are appearing. In September a spate of nine incidences of synthetics harm in south Taranaki was the most recent point of focus.
In terms of acute harm, synthetic cannabinoids are “the worst drugs in this country,” says an analyst from High Alert, an early warning system which tracks which drugs are circulating in the country. High Alert provides alerts or warnings if a particularly harmful substance is being bought and sold. It is led by the National Drug Intelligence Bureau and supported by a range of community and government partners that regularly encounter and respond to drug-related harm.
“It's not one of the more common drugs we see, but when you look at acute harm, when you could have one bong and never wake up, synthetic cannabinoids are the worst.”
Police are also part of this network, and in 2019, Police and Customs seized 23.5kg of synthetic cannabinoids — a steady decrease from a peak of over 200kg in 2016. These seizures were made up of both powder and prepared plant material.
“Given the serious harm that occurred over 2017-2019, it’s almost certain this reduction in supply prevented numerous instances of synthetic cannabinoid-related harm and likely saved lives,” Detective Inspector Blair MacDonald says.
Resources, training and constant communication are all part of the plan to stop synthetic cannabinoids from causing more harm, as is money available from a contestable government fund established so affected communities can ask for financial help as and when problems relating to the substances appear in their communities.
And with High Alert up and running there is a national focal point for information distribution. This way, if there is one location or one strain causing concern, High Alert can “sound the alert and work with our network partners to formulate a health-based response,” MacDonald says. Involving the news media at this point is part of that plan.
Part of the toolkit developed for combating harm is training Emergency Department staff to notice if people turn up presenting behaviour known to be associated with synthetic cannabinoid use. When that happens, blood and urine samples can be requested, as well as requests for any substance the person might have on them, which will then be sent for testing.
These chemicals are often so new, that their medical effects are unknown or only anecdotal."
Hannah PartingtonA surge in reports of synthetic cannabinoids is not a surprise according to Emily Hughes of the Drug Foundation. After new strains enter the black market, there can be a delay before these are classified as banned substances. Once banned, the production, importation and sale of these substance attracts higher penalties. Therefore black market operators have an incentive to continually bring in new ones.
Lack of access to cannabis is also thought to be a driver as to whether a country has a synthetics problem: in countries where cannabis is legal, the need to access synthetic alternatives is much lower.
There is also incentive to make new synthetic products as potent as possible, so that smaller quantities overall need to be imported. It can be hard to tell the strains apart, says Institute of Environmental Science and Research (ESR) forensic chemist Hannah Partington.
“This becomes a very real problem for the user who is likely to have no idea what they are consuming and how much of the synthetic cannabinoid is present. In addition, these chemicals are often so new, that their medical effects are unknown or only anecdotal,” Partington says.
Justin Clinton-Gohdes, the mental health and addictions manager at the Taranaki DHB, says he feels confident the current presence of synthetic cannabinoids in the district will not become as harmful as last time, due to the work put in in the intervening months by the acute drug harm response network.
Hughes says it’s important to inform people using drugs of different synthetic cannabinoid strains, and what to look out for. “Dropping”, where someone using synthetics loses consciousness, had become normalised amongst those who use the substance, which is worrying.
“For example if everyone is using together and one or two might fall unconscious and people think ‘oh that's what he normally does’ and then four hours later it turns out he’s been dead the whole time. Our advice is if someone does appear to fall asleep, to check they are still breathing and call 111 if they are not responsive or are struggling to breath,” Hughes explains.
Because synthetic cannabinoid use tends to concentrate in low socioeconomic areas, officials are mindful that stresses associated with Covid-19 (job loss, loss of secure housing) could create increased demand for the substance.
A spokesperson for Lifewise says wraparound services are needed, to stop people from getting into situations where they seek synthetics. “Lifewise advocates for a more holistic, whānau-led, iwi-led approach to harm reduction and addressing the ill effects of addiction.”
For now, organisations like High Alert are keeping their eyes peeled.
“It’s a core crux of High Alert to have our finger on the pulse if it does happen. If it spreads to Palmerston North, if it spreads to Wellington, we will be there to warn people,” MacDonald says.
Recent news

Reflections from the 2024 UN Commission on Narcotic Drugs
Executive Director Sarah Helm reflects on this year's global drug conference
What can we learn from Australia’s free naloxone scheme?
As harm reduction advocates in Aotearoa push for better naloxone access, we look for lessons across the ditch.

A new approach to reporting on drug data
We've launched a new tool to help you find the latest drug data and changed how we report throughout the year.

